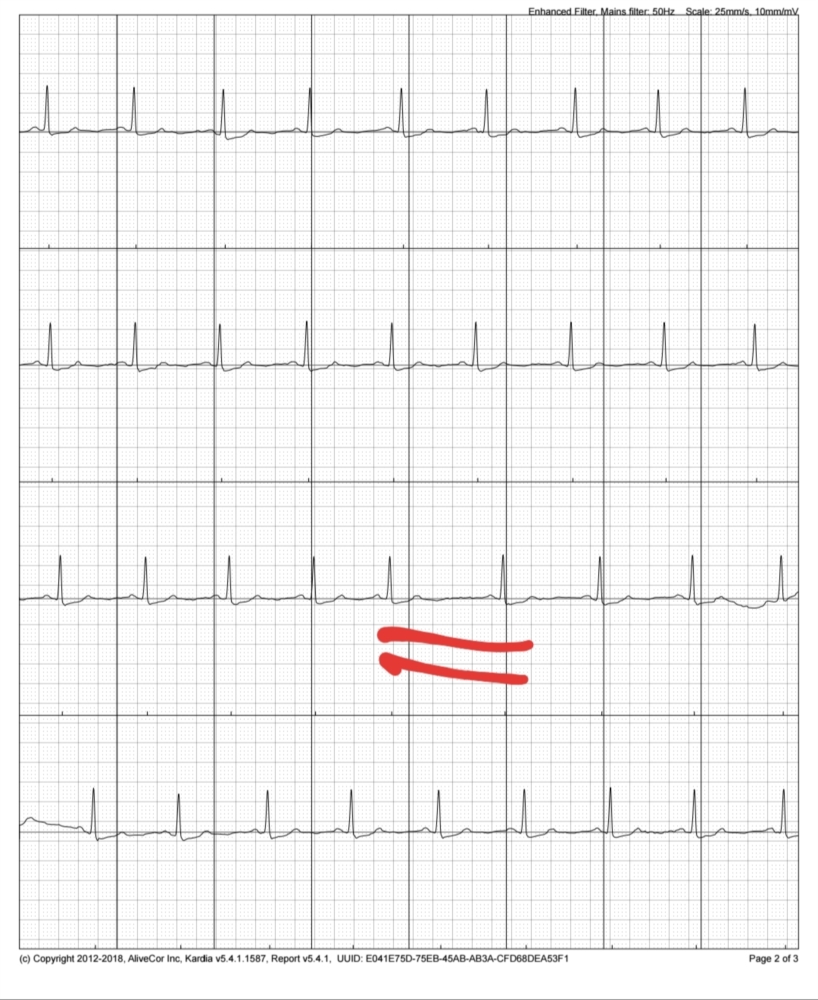
No acute distress, no skin changes or rashes, no elevation in jugular venous pressure, and no carotid bruits. Physical examination: Pulse 72 beats per minute – regular and equal in both arms, blood pressure in left arm 130/85 mm Hg and 135/85 in the right arm. Patient denies any consumption of alcohol, illicit drugs, or supplements. Patient does not have significant family history of heart disease, diabetes, cancer, or congenital abnormalities, and he is compliant with yearly preventive visits to his primary physician. His medical history is significant for obesity (BMI = 34), treated hypertension (on hydrochlorothiazide 25 mg orally once daily), treated obstructive sleep apnea (he was seen at a sleep medicine center nine years ago, and he has been using a continuous positive airway pressure device every night since then), and history of tobacco use (15 pack/year history he completely quit smoking 12 years ago). The patient denies any episodes of syncope, pre-syncope, chest pain, shortness of breath, or significant changes in exercise tolerance, temperature tolerance, or any recent changes in medications. On further questioning he notes similar episodes of palpitations occurred earlier this year, approximately three times: all of them resolved spontaneously after one to three hours, and he did not seek medical attention for them. Read his story.A 47-year-old Caucasian man presents to an outpatient appointment with abrupt onset of mild palpitations that occurred the same morning when he woke up, and lasted for 50 minutes during which the patient felt mild malaise. Frank had an ablation to treat atrial flutter and is still playing golf four times a week.  
If this happens you may wish to speak to your loved ones and your GP for further support. You may be feeling more anxious or stressed than normal after your diagnosis. Living with atrial flutter can also have an emotional impact on you and your family. However, it can take time to understand what triggers your atrial flutter and you may need to make some changes. With treatment, you should continue to do everything you enjoy after your diagnosis. To reduce this risk of having a stroke, you may need to take an anticoagulant medicine, such as warfarin or a NOAC. If the clot breaks off it could lead to a stroke. This can lead to a blood clot forming in your heart. medicines to control your heart rate such as beta blockers, calcium channel blockers and other anti-arrhythmic medicines.Ītrial flutter can cause blood to pool in your ventricles.Your doctor might recommend treatment with: You may also have an electrophysiological (EP) study to look at the electrical signals in the heart more closely. Your doctor should recommend you have an ECG or Holter monitor to look at your heart rhythm. The top part of the heart beats quicker than the bottom, causing an abnormal heart rhythm. This causes the atria to twitch, leading to an abnormal heart rhythm.Ītrial flutter is when the atria beat regularly, but much faster than usual. What's the difference between atrial flutter and atrial fibrillation?Ītrial fibrillation is when the atria beat irregularly. Some people with atrial flutter may also have atrial fibrillation and experience periods of atrial flutter followed by periods of atrial fibrillation. Sometimes atrial flutter can occur without any cause. another condition, such as lung disease or overactive thyroid.inflammation of the heart (such as myocarditis).People with atrial flutter often have an underlying heart or circulatory condition such as: If you're experiencing any of these symptoms, especially if you already have a heart condition, speak to your GP. Although people with atrial flutter often have no symptoms, symptoms can include:
0 Comments
Leave a Reply. |
 RSS Feed
RSS Feed
